Migraines in Women: A Focus on Reproductive Events and Hormonal Milestones
Article information
Abstract
Migraine, a prevalent neurological disorder, is more common in women than in men. This sex difference is more pronounced after menarche and diminishes after menopause. Migraines in women are influenced by the menstrual cycle, pregnancy, and lactation, suggesting a connection to sex hormones, known as the estrogen withdrawal theory. Beyond endogenous hormonal changes accompanying reproductive events, exogenous hormonal factors such as contraceptives or hormone replacement therapy may also affect migraines. The hormonal influence cannot be explained simply by serum estrogen levels; instead, it involves a complex interplay of various factors. Here, we delineate aspects of migraines associated with endogenous and exogenous hormonal changes over the course of a woman’s life, exploring the mechanisms and contributing factors through which sex hormones influence migraines.
INTRODUCTION
Migraines are a prevalent neurological disorder that significantly affect daily life and pose substantial socioeconomic burdens. More than 10% of the general population experiences migraines, with a higher prevalence reported among women.1 Sexual differences in migraine prevalence become more pronounced after puberty and decrease after menopause, and sex hormones are known to play a role.2 The well-established phenomenon of menstrual migraine, which is characterized by headaches induced by a decrease in estrogen levels during the late luteal phase, is known as the “estrogen withdrawal theory.”3 Estrogen also plays a crucial role in modulating excitatory and inhibitory pain neurotransmission.4 These findings suggest that hormonal factors can significantly influence the sexual differences observed in migraine.
Women experience various endogenous and exogenous reproductive events, including menstruation, pregnancy, breastfeeding, menopause, contraception, and hormone replacement treatment (Figure 1). These events can induce rapid and variable changes in hormonal status, potentially influencing migraine symptoms and prevalence. Consequently, understanding the association between hormones and migraines will be essential to any investigation of the mechanisms and treatment of migraines. This review describes the intricate relationship between migraines and hormones in women. Also, this review describes the hormonal changes in response to reproductive events throughout a woman’s life and how these changes contribute to patterns in migraine occurrence.
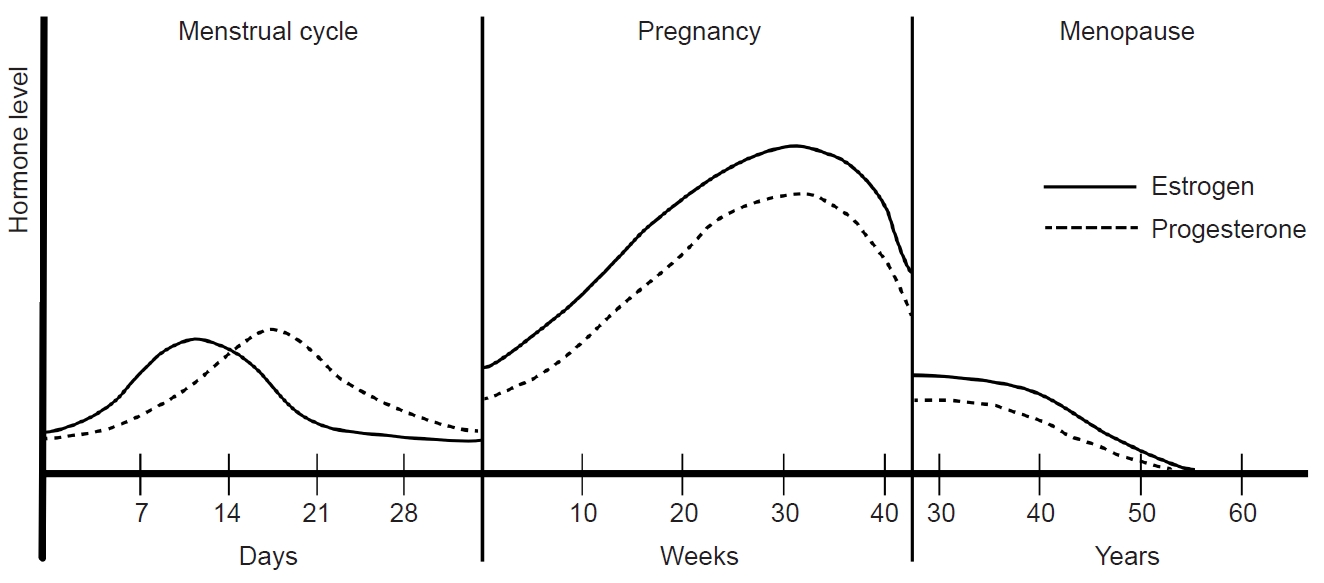
A fluctuations in women’s sex hormones across life stages. Women experience fluctuations in sex hormones with reproductive events throughout their lives. After menarche, cyclical fluctuations in estrogen and progesterone occur with menstruation. During pregnancy, estrogen and progesterone remain elevated, normalize after childbirth, and decrease during menopause.
SEX DIFFERENCES IN MIGRAINE EPIDEMIOLOGY AND SYMPTOMS
The prevalence of migraines is reportedly three times higher in women than in men.5 According to the American Migraine Prevalence and Prevention study, the overall 1-year migraine prevalence is of 11.7%, with women experiencing a prevalence of 17.1% compared with 5.6% in men. The cumulative incidence was 43% in women and 18% in men.1,5 Another study, utilizing National Health Interview Survey data, reported a prevalence of 13.2% in the general population, with rates of 17.5% in women and 8.6% in men.6 In a Korean nationwide cross-sectional survey, structured interviews with 1,507 subjects conducted by trained interviewers showed a 1-year migraine prevalence of 6.1% in the overall population, 9.2% in women, and 2.9% in men.7 These findings consistently show that migraines are more common in women than in men.
Sex differences in migraine prevalence vary across age groups. Studies of pediatric migraines reported a prevalence of 4%, with no sex differences before puberty, and an increase in women older than 11 years.8,9 The migraine prevalence was 4.0% in men and 6.4% in women aged between 12 and 17 years and it was highest among those 30–39 years of age for both sexes (24.4% in women; 7.4% in men) and lowest after the age of 60 years (5% in women; 1.6% in men). The difference in migraine prevalence between sexes was highest in the 30–39 age group.1,5 Previous study revealed a bimodal peak in 1-year migraine prevalence at 20 and 50 years for both sexes. After the age of 10 years, migraine prevalence was consistently higher in women than in men. The difference in prevalence was greatest at age 30.2 years, with a 2.9-fold difference, and remained about 2-fold after the age of 42 years.6
Women with migraines tend to experience migraines for longer durations, at greater frequency, and in closer association with photophobia, phonophobia, nausea, and vomiting, compared with men.10-13 The impact of sex on migraines becomes more significant after the age of 30 in women.10 Although there is no significant difference in migraine medication use according to sex, women with migraines are more likely than men to take both acute and preventive medications.14 Prognostically, a previous study reported that 23% of pediatric migraines resolve before the age of 25, with a higher resolution rate in men (34%) than in women (15%). By the age of 50 year, 46% were migraine-free, with no significant sex difference.8
ROLES OF SEX HORMONES IN MIGRAINE
Sex differences in migraine prevalence emerge at puberty when women begin to menstruate and experience periodic hormonal changes during the menstrual cycle. Estrogen and progesterone are known to be related to migraine pathophysiology. Gonadotropin-releasing hormone (GnRH) from the hypothalamus stimulates the secretion of luteinizing hormone (LH) and follicular stimulating hormone (FSH) from the pituitary. LH and FSH trigger ovarian maturation and ovulation, promoting the secretion of estrogen and progesterone, which are regulated by feedback mechanisms.15 Sex hormones have low molecular weights and lipophilic properties, allowing them to passively diffuse across the blood-brain barrier. Consequently, central and peripheral levels of sexual steroid hormones are comparable, exerting an influence on migraines through neurotransmitter and pain modulation systems.16,17 However, the effects of sexual steroid hormones on migraines are complex, with mixed effects reported depending on the site of action, duration, and concentration.
1. The impact of sex hormones on the neurotransmitter system
Several neurotransmitter systems, including serotonin (5-hydroxytryptamine [5-HT]), noradrenaline, gamma-aminobutyric acid (GABA), opioids, and glutamate have been implicated in the pathophysiology of migraines. Sexual steroid hormones play a crucial role in the regulation of these neurotransmitter systems.
Serotonin is a neurotransmitter associated with migraines, and an increased serotonin synthesis capacity has been observed in migraine patients.17 Triptans, which are commonly used to treat migraines, are selective serotonin receptor agonists (5-HT1B, 5-HT1D). Tryptophan hydroxylase (TPH) is the rate-limiting enzyme for serotonin synthesis, and a previous study on oophorectomized monkeys reported that TPH mRNA activity increased nine-fold with estrogen supplementation and five-fold with an estrogen-progesterone combination.18 The serotonin reuptake transporter (SERT) at the presynaptic area is responsible for serotonin reuptake and degradation. In oophorectomized monkeys, short-term estrogen supplementation (<28 days) decreased SERT mRNA activity.19,20 Monoamine oxidase (MAO) is the primary enzyme that degrades serotonin. Estrogen decreases the expression of MAO genes in the hypothalamus and dorsal raphe nucleus.21 These findings suggest that estrogen increases serotonergic activity and potentially promotes migraine symptoms. Progesterone may have fewer influences on the serotonin system, and the serotonergic system may respond differently based on the duration of estrogen supplementation.
The noradrenergic system plays a crucial role in modulating the signal-to-noise ratio of neurons in response to incoming afferent stimuli. Estrogen is known to increase the gene expression of tyrosine hydroxylase, the rate-limiting enzyme in noradrenaline biosynthesis.22 In animal studies, estrogen infusion elevated noradrenaline secretion in the mediobasal hypothalamus and enhanced the gene expression of tyrosine hydroxylase in the locus coeruleus.23 Glutamic acid, an excitatory neurotransmitter linked to pain transmission, is also influenced by estrogen. Acute exposure to estrogen increases the glutaminergic neuronal firing of hippocampal Purkinje cells, while chronic exposure enhances dendritic spine density and excitatory synapses of hippocampal glutaminergic neurons.17
Glutamic acid decarboxylase is responsible for converting glutamate to GABA, an inhibitory neurotransmitter, and shows increased activity with estrogen. This results in heightened GABA release and up-regulation of GABA receptors.24 Estrogen injections can also increase enkephalin mRNA activity in the spinal cords of female rats. Both estrogen and progesterone contribute to an increased binding affinity of kappa-opioid receptors in oophorectomized rats.25-27 These findings emphasize the intricate influence of sexual steroid hormones on various neurotransmitter systems and their potential role in modulating neuronal responses and pain pathways.
2. Calcitonin gene-related peptide and sex differences in migraines
Calcitonin gene-related peptide (CGRP) is a key pathophysiological factor in migraines. It is released in the brain and influences pain transmission within the trigeminal nervous system. During a migraine attack, CGRP levels increase jugular blood flow, which subsequently decrease after migraine symptoms improve in response to administration of sumatriptan.28,29 An intravenous CGRP injection can trigger migraine attacks in 65% of migraine patients but not in control groups, implying that the former may possess a lower threshold to CGRP.30-32 Clinically, CGRP receptor antagonist and monoclonal antibodies against CGRP are employed in migraine treatment.
Several studies suggest a potential association between CGRP and sex differences in migraines. The administration of dural CGRP induces a decrease in the facial withdrawal threshold to mechanical stimuli in female rats but not in male rats. Intracisternal injections of brain-derived neurotrophic factor, and interleukin-6 decrease the facial withdrawal threshold in rats, which recover after 72 hours, and subsequent dural CGRP administration delays the recovery response only in female rats.33 In both sexes, administration of CGRP to the trigeminal ganglion results in a decrease in the threshold of mechanical stimuli, but recovery of mechanical allodynia with minocycline and propentofylline was observed only in male rats.34 CGRP induces vasodilation of meningeal vessels, a process linked to migraine pathophysiology.35 A study investigating vasodilation responses in ovariectomized rats found that estradiol premedication increased vasodilation in responses to electrical stimulation. In meningeal arterial system, estradiol increases the CGRP-immunoreactive sensory innervation and promotes release of CGRP from nerve endings innervating the meningeal artery.36
Transient receptor potential ankyrin 1 (TRPA1), and transient receptor potential melastatin 8 (TRPM8), both of which are transient receptor potential channels of trigeminal neurons, are closely related to migraine pathophysiology. TRPA1, found on the primary afferent neurons innervating the meninges, releases CGRP when activated. Nitroglycerin increases TRPA1-mediated neuronal activity, promoting nociceptive hypersensitivity. TRPM8 attenuates migraine symptom and TRPA1-related pain. The antinociceptive action of TRPM8 is more pronounced in male rats and necessitates testosterone. Exogenous testosterone induces the recovery of mechanical hypersensitivity in female and orchiectomized male rats, implying potential sex-dependent effects of TRPM8 on migraines.37
Interplay between prolactin and CGRP may contribute to sex differences in migraines. Although serum prolactin levels do not differ between migraineurs and controls, prolactin increases during a migraine attack but not in tension-type headaches.38,39 Dural prolactin administration decreases the withdrawal threshold for mechanical stimuli in female rats but not in male rats. An immunohistochemical analysis reveals a prolactin receptor in the dural afferent nerve of female rats but not in male rats. Prolactin stimulates the release of CGRP and activates the dural trigeminal ganglion neurons only in female rats.40
MENSTRUATION AND MIGRAINES
1. Menarche, menstruation, and hormonal dynamics
Menarche marks the onset of the first menstrual period in women, and in Korea, the mean age of menarche is reportedly 12.9±1.18 years.41 Following menarche, approximately 10 anovulatory menstrual cycles occur per year, with a serum estrogen level ranging from 10 to 156 pg/mL. Over subsequent years, the serum estrogen level gradually aligns with that of an adult.42 This transition period signifies the maturation of the reproductive system and involve adjustments in hormonal levels and menstrual cycle characteristics.
The menstrual cycle can be divided into two main phases: the follicular phase and the luteal phase, as determined by the occurrence of ovulation. The follicular phase spans from the onset of menstrual bleeding to just before ovulation, while the luteal phase extends from ovulation to the commencement of the next menstrual cycle. With an average duration of 28 days, a menstrual cycle is characterized by a constant luteal period of 14 days, and the entire cycle is predominantly influenced by the follicular phase. In the follicular phase, FSH and LH stimulate follicle maturation and estrogen secretion, respectively, in the ovary. The early follicular period sees low serum estrogen levels ranging from 25 to 50 pg/mL, with progesterone levels remaining below 1 ng/mL. As the follicular phase progresses, estrogen levels rise steadily, reaching a peak of 100 to 400 pg/mL during the late follicular to early luteal periods. This estrogen surge triggers the abrupt secretion of LH, leading to ovulation.
In the subsequent luteal phase, the corpus luteum, a temporary endocrine structure formed after ovulation, produces both estrogen and progesterone. During this phase, estrogen inhibits GnRH, FSH, and LH, while progesterone plays a crucial role in maintaining the endometrium of the uterus. In the absence of fertilization, serum estrogen levels remain between 200 and 300 pg/mL throughout the luteal period, decreasing to 25–50 pg/mL before the onset of the next menstrual cycle. Concurrently, serum progesterone levels increase to 6–10 ng/mL during the mid-luteal period and decrease to 2 ng/mL in the late luteal period. These intricate hormonal dynamics orchestrate the menstrual cycle, regulating the physiological processes essential for reproductive health (Figure 2).
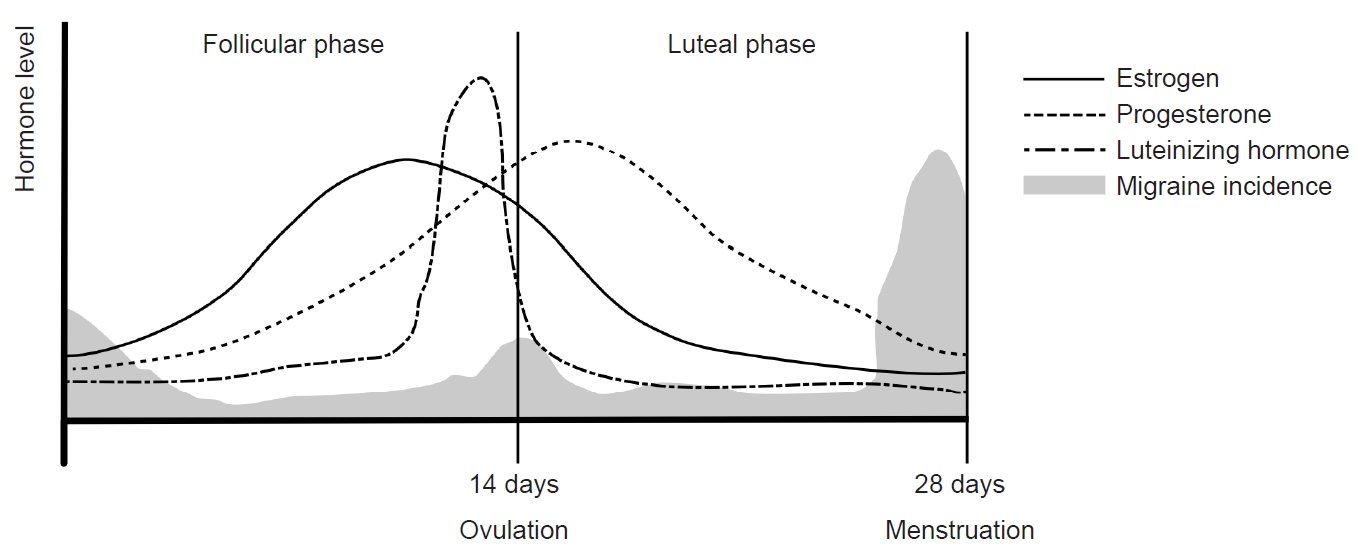
Hormonal changes and menstrual migraine during the menstrual cycle: The menstrual cycle can be divided into follicular and luteal phases according to ovulation. Following ovulation, the corpus luteum produces estrogen and progesterone. In the absence of fertilization, estrogen secretion decreases, leading to the initiation of menstruation. Menstrual migraines occur during the period from 2 days before to 3 days after menstruation.
2. Menstrual migraine and estrogen withdrawal theory
A menstrual migraine is defined as a migraine that occurs from two days before to three days after the onset of menstruation. Previous studies have reported that menstrual migraines often peak 2 days before menstruation and are not associated with ovulation.43,44 Additionally, there is a reported connection between serum estrogen levels and menstrual migraines. These migraines frequently occur during the late luteal and early follicular periods when serum estrogen levels decrease rapidly. In contrast, migraine attacks are less frequent when serum estrogen levels are stable.45 For individuals with migraines, attacks during the perimenstrual period tend to be more severe and last longer compared with other phases of the menstrual cycle.46,47 Although the mean serum estrogen level does not differ significantly between migraineurs and those without migraines, migraineurs exhibit a more rapid decline in estrogen during the luteal period compared with controls.48
These findings support a close relationship between estrogen decline and migraines, which underlies the estrogen withdrawal theory. In the late luteal period, estrogen supplementation has been shown to delay migraine attacks, while progesterone does not exert the same effect.49,50 However, during the mid-follicular phase, migraines reportedly did not occur when short-acting estrogen was administered to induce a change in estrogen concentration. This suggests that priming of estrogen may be necessary before actual estrogen withdrawal triggers migraines.51
3. Difference in menstrual migraine between migraines with and without aura
An interesting distinction in menstrual migraine has been observed between individuals with migraine without aura (MO) and those with migraine with aura (MA). In a study examining headache patterns during the menstrual cycle in 81 women with migraines, menstrual cycles were divided into five study periods (3–7 days before menses, 1–2 days before menses, 0–1 days after menses, 3–5 days after menses, and 14–15 days before menses) and a control period. The study found that the risk of MO increased in the period 1–2 days before menses (odds ratio [OR], 2.04; 95% confidence interval [CI], 1.49–2.81), and the period 0–1 day after menses (OR, 1.80; 95% CI, 1.40–2.30). However, the risk of MA did not differ significantly among study periods.52 Another study investigated the differences in migraine symptoms between perimenstrual and non-perimenstrual migraines in women with migraines. Perimenstrual migraine headaches were found to have a longer duration, higher recurrence risk, increased triptan intake, higher headache intensity, and more pronounced photophobia and phonophobia compared with non-perimenstrual headaches. However, the prevalence of aura was lower in perimenstrual headaches (OR, 0.8; 95% CI, 0.6–1.0).46 A further investigation into perimenstrual migraine differences between women diagnosed with MO and MA revealed that, while the prevalence of migraine attacks did not differ between the two groups (59% for MO versus 53% for MA, p=0.176). The risk of migraine attack without aura was significantly higher during the perimenstrual period in both MO (OR, 1.53; 95% CI, 1.44–1.62) and MA groups (OR, 1.53; 95% CI, 1.44–1.62). However, the risk of MA attacks did not show a significant change within the perimenstrual period (OR, 1.08; 95% CI, 0.93–1.26). This implies that the most common form of perimenstrual migraine is MO, even in individuals diagnosed with MA (Figure 3).53 The cause of these differences is unclear but may be related to variations in the effects of estrogen on the trigeminal-vascular system and cortical spreading depression (CSD). In migraine patients, headache occurrence is related to the trigemino-vascular system and is caused by the short-term effects of estrogen. In CSD, the occurrence of aura is thought to be related to the long-term effects of estrogen.54 An animal study investigating the association between estrogen and CSD found that CSD was more frequently observed in female rats than in male and ovariectomized female rats. In female rats, the risk of CSD remained unchanged during normal menstrual cycles and with long-term (3-week) estrogen supplementation. However, when the rats underwent 2 weeks of estrogen treatment followed by 1 week of withdrawal, the incidence of CSD increased.55 This study suggests that the development of CSD is not directly linked to estrogen withdrawal during the natural menstrual cycle. Instead, it appears to be associated with withdrawal after a prolonged period of estrogen exposure.
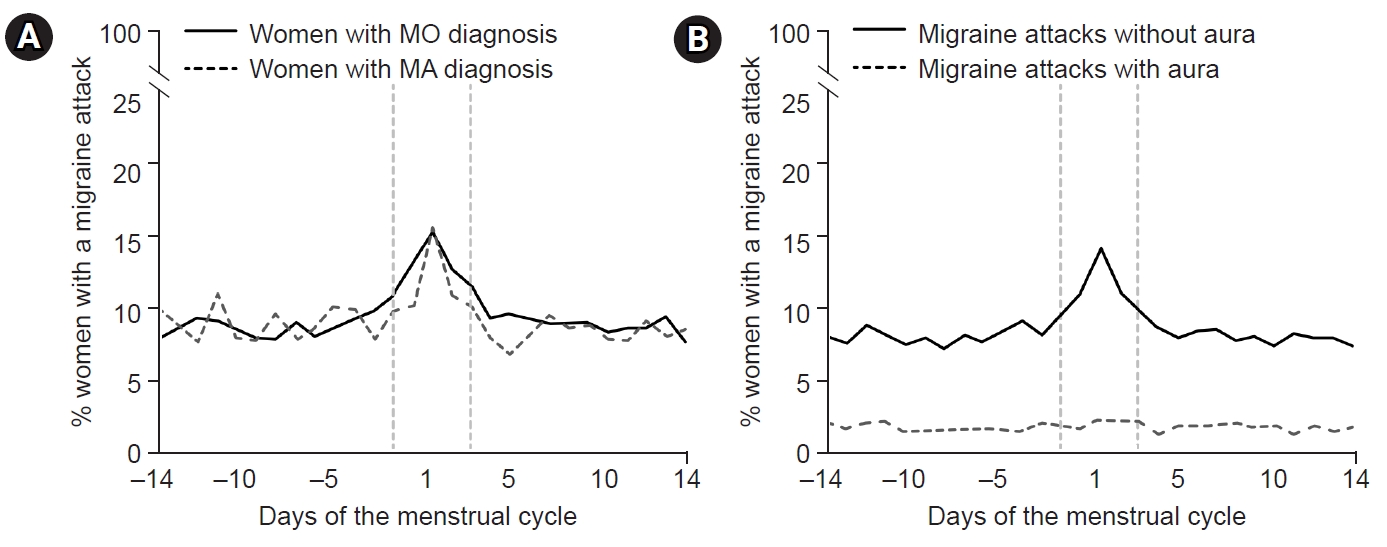
Differences in perimenstrual migraines between women diagnosed with migraines without aura (MO) and migraines with aura (MA): (A) The prevalence of migraine attacks did not differ between women with MO and MA. (B) The risk of MO was significantly higher during the perimenstrual period in all groups of women with migraines. Modified from Verhagen et al. (Cephalalgia 2023;43:3331024231164322).53
PREGNANCY, LACTATION, AND MIGRAINES
During pregnancy, the consistent production of estrogen and progesterone by the placenta results in a stable hormonal environment free from the fluctuations of the menstrual cycle. In the third trimester, levels of serum estrogen (30–40 times) and progesterone (20 times) are significantly elevated compared with the peak levels in the menstrual cycle.56 Following childbirth, the hormonal status and menstrual cycles vary depending on whether lactation occurs. Prolactin, a pituitary hormone associated with lactation, maintains a serum level of 10–25 ng/mL before pregnancy. During pregnancy, estrogen and progesterone promote mammary gland maturation while inhibiting prolactin secretion and lactation. Within 24 hours postpartum, serum estrogen and progesterone decrease, and prolactin increases, initiating lactation (Figure 4).57
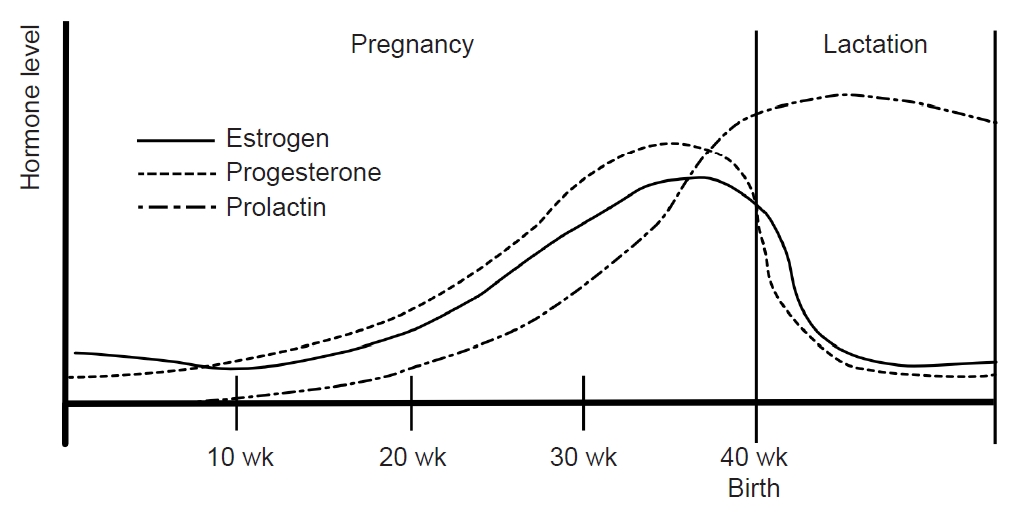
Sex hormones during pregnancy and lactation: During pregnancy, estrogen and progesterone remain at high levels without fluctuating. Immediately after childbirth, estrogen and progesterone decrease and prolactin increases. During lactation, prolactin is maintained at a high concentration and inhibits the secretion of estrogen and progesterone. Their concentrations remain low without fluctuations.
Pregnant women with a history of migraines reportedly show significant improvement in the second and third trimesters, with improvement rates of 46.8% in the first trimester, 83% in the second trimester, and 87% in the third trimester. Some women even experience complete remission of migraines during pregnancy, with remission rates of 11% in the first trimester, 53% in the second trimester, and 73% in the third trimester. Notably, many of these changes in migraine patterns during pregnancy revert to their previous state after childbirth.58
These changes in migraines during pregnancy are likely associated with hormonal influences. The continuous high and steady serum estrogen levels during pregnancy align with the estrogen withdrawal theory, which posits that stable estrogen levels lead to migraine improvement. The reversion of migraine patterns after childbirth supports this hypothesis.59-61 Another potential mechanism involves the influence of pregnancy on pain transmission. Animal studies have shown that both the nociceptive threshold and dynorphin increase in the lumbar spinal cords of pregnant rats. Simulated pregnancy in animal models using estrogen and progesterone demonstrated similar opioid analgesia in the spinal cord.27
However, some women without a previous history of migraines experience new-onset migraines during pregnancy, with occurrence rates of 1.3% to 18%. This phenomenon is predominantly associated with MA. It is more prevalent during the first trimester and is believed to be related to a rapid increase in estrogen levels rather than estrogen withdrawal.58,59
During lactation, mechanical breast stimulation enhances prolactin production. Prolactin inhibits the release of GnRH, suppressing estrogen and progesterone release and preventing ovulation.57 Subsequently, serum estrogen levels remain consistently low without fluctuations in lactating women (Figure 4). Clinical studies have found that most women who bottle-feed their children experience migraine recurrence within 1 month after delivery compared with only 43.2% of breastfeeding women.58 In women who bottle-feed, the decrease in prolactin restarts the menstrual cycle, leading to hormonal fluctuations that can increase the frequency of migraines.57
MENOPAUSE AND MIGRAINES
Menopause is the cessation of menstruation for more than 1 year without other identifiable causes. The mean age of menopause is approximately 50 years, with a reported mean menopausal age in Korea of 49.3±3.5 years.62 Distinct effects on migraines have been observed between menopause and the perimenopausal period.
A woman’s ovarian follicles are limited in number, with most producing approximately 400–500 ova over 40 years, after which ovarian function diminishes. Women typically experience an irregular menstrual cycle for 2–8 years before entering menopause, a stage known as perimenopause and characterized by a decline in ovarian function. During this phase, women experience hypergonadotropism, hypoestrogenism, hypoprogesteronism, and greater estrogen fluctuations.63 The excessive stimulation of remaining follicles results in severe estrogen fluctuations. After menopause, serum estrogen and progesterone levels remain consistently low without fluctuation.64 According to the estrogen withdrawal hypothesis, estrogen fluctuations during perimenopause can contribute to frequent migraine attacks, with an anticipated improvement in migraines after menopause.
A cross-sectional study reported an increase in migraine prevalence during perimenopause, followed by a decrease after spontaneous menopause. However, this study focused on women aged 40 to 54 years and did not comprehensively analyze postmenopausal women.65 Another study indicated an increased risk of migraines in perimenopausal woman (OR, 1.42; 95% CI, 1.03–1.94) but not significantly in postmenopausal women (OR, 1.27; 95% CI, 0.83–1.92) compared with premenopausal women.66 These findings support the exacerbation of migraines during the perimenopausal period, although the effect of menopause on migraines remains inconclusive.
While some studies have reported a decrease in migraine prevalence after menopause, others found no significant differences among premenopausal, perimenopausal, and postmenopausal periods.67-69 In women with migraines, improvement after menopause ranges from 8%–36%, worsening from 9%–42%, and remaining unchanged from 27%–64%. Additionally, 8%–13% of women may experience their first migraine after menopause.15 Other clinical factors may affect postmenopausal migraines. The risk of migraines risk in cases of early artificial menopause, such as those associated with a hysterectomy or oophorectomy, with a higher risk has been reported in surgical menopause compared with spontaneous menopause. Previous studies reported a migraine risk of 27% in surgical menopause but 7% in spontaneous menopausal women.64,65,70 Previously, we reported that a shorter lifetime number of year of menstruation (LNYM) and hormone replacement therapy (HRT) may contribute to an increased risk of migraines in postmenopausal women.71 The LNYM represents the cumulative duration of menstruation cycles and cumulative exposure to endogenous hormones over a women’s life.72,73 Our study suggests an elevated risk of postmenopausal migraine in women with either exogenous hormone exposure or insufficient endogenous hormone exposure.
The long-term incidence of migraines after menopause has not been fully elucidated. In a previous study utilizing the Korean National Health Insurance Service database, we reported that the risk of migraines was higher in women in longer postmenopausal groups, including those postmenopausal for ≥15 years (HR, 1.196; 95% CI, 1.169–1.224), <15 years (HR, 1.09; 95% CI, 1.069–1.111), and <10 years (HR, 1.042; 95% CI, 1.027–1.058) compared with the <5 years group. Our results suggest that an extended period after menopause may increase the risk of migraines again.71 The mechanism is unclear, but it is possible that prolonged low estrogen levels may lower pain thresholds due to decreased GABAergic and opioidergic effects of estrogen.
EXOGENOUS HORMONAL FACTOR (CONTRACEPTION AND HORMONE REPLACEMENT THERAPY) AND MIGRAINES
In women, physiological processes such as menstruation, pregnancy, and lactation represent endogenous hormonal changes, while contraception and HRT introduce exogenous hormonal alterations. Male-to-female transsexuals taking estrogen often experience heightened and exacerbated headaches.74 Conversely, some prior studies have indicated that continuous estrogen or HRT may alleviate headache symptoms, suggesting a potential influence of exogenous estrogen on migraine.60,75 The impact of exogenous hormones on migraines can vary based on type, composition, timing, and route of administration.
Contraception is commonly utilized to manage menstrual cycles and prevent pregnancy, with various administration methods available. This discussion focuses on combined oral contraceptives (COCs), the most frequently used form. The notion that COCs increase the prevalence of migraines and worsen migraine symptoms is generally accepted.15 Approximately 70% of women who experience migraines report exacerbation of symptoms with COCs.76 This exacerbation tends to be more pronounced in women with MA compared with those with MO, and the frequency of auras often increases.60 These exacerbations are frequently observed during pill-free periods, with a four-fold increase in the prevalence of migraine attacks on pill-free days 3–6.77
Among women without a history of migraine, COC use has been associated with a significant increase in migraine prevalence (OR, 1.4; 95% CI, 1.2–1.7) compared with those who have never used COCs.78 However, conflicting findings exist, with other studies reporting that migraine headache patterns remained unchanged in 44%–67%, worsened in 24%–36%, and improved in 5%–8% with the use of COCs.79-81 Another study suggested that continuous estrogen administration could decrease the symptoms and frequency of migraines.60 These discrepancies in the effects of COCs on migraines can be attributed to differences in the composition and dosage of COCs, with recent research suggesting that low-dose estrogen pills have a reduced impact on migraines.15
After menopause, women experience various postmenopausal symptoms, such as hot flushes, irritability, insomnia, mood changes, and osteoporosis. HRT is commonly used to alleviate menopausal symptoms and may involve estrogen alone or in combination with progesterone.15 The effects of HRT on migraines remain inconsistent across studies. In one study investigating changes in migraine symptoms during HRT, migraine symptoms worsened in 21%, improved in 22%–23%, and remained unchanged in 57% of migraineurs.82 Another study reported that migraine symptoms did not change in 77% of migraineurs with HRT.80 In a population-based study, headache prevalence increased in women who did not have a history of headaches.75 Another population-based study of 17,107 postmenopausal women reported that current HRTs significantly increase the risk of migraine (OR, 1.42; 95% CI, 1.24–1.62) compared with a non-HRT population.83
Differences in HRT composition and administration methods can influence its effects on migraines. Continuous estrogen administration is associated with a decrease in migraine severity and attack frequency.60 Non-oral estrogen may have a more favorable impact on migraines compared with oral administration.84 For example, in one study, users of transdermal estradiol patches did not experience changes in headache symptoms, while headaches worsened in those receiving oral HRT.85 However, a population-based cross-sectional study reported that the routes of HRT administration were not associated with migraine risk, while an HRT group had a greater migraine risk compared with the non-HRT group.86
In summary, COCs are generally associated with migraine exacerbations, and low-estrogen pills may have a reduced impact on migraines. HRT also tends to exacerbate migraines, but the effects are influenced by composition, dose, and route of administration.
CONCLUSION
Women’s migraines are profoundly influenced by hormonal changes, and the dynamic nature of hormonal fluctuations throughout their lives contributes to the complexity of this relationship. The same hormone can elicit opposite effects on migraines depending on the timing, dose, and other factors. It is therefore important to understand the fluctuations in female hormones and how they affect migraines at different times. In addition to exploring previous neurotransmitter systems, recent studies investigated CGRP as a potential mechanism underlying hormonal effects on migraines. These studies contribute valuable insights into the intricate interplay between hormonal dynamics and the manifestation of migraines. Understanding the effects of hormones on migraines is a crucial aspect of research into the mechanisms of migraines and their treatment.
Notes
Availability of data and material
Not applicable.
Author contributions
Conceptualization: JWP; Data curation: SK; Investigation: SK; Writing–original draft: SK; Writing–review and editing: JWP.
Conflict of interest
No potential conflict of interest relevant to this article was reported.
Funding statement
Not applicable.
Acknowledgements
Not applicable.
